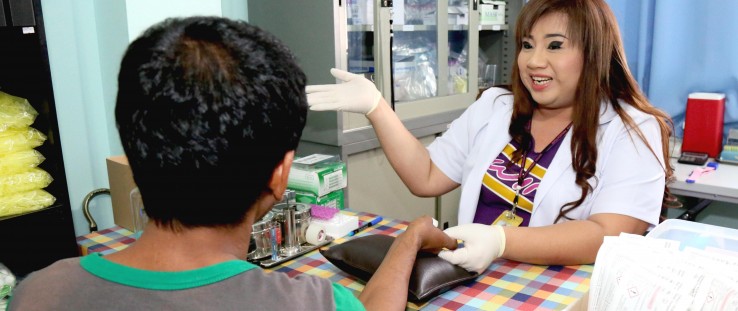
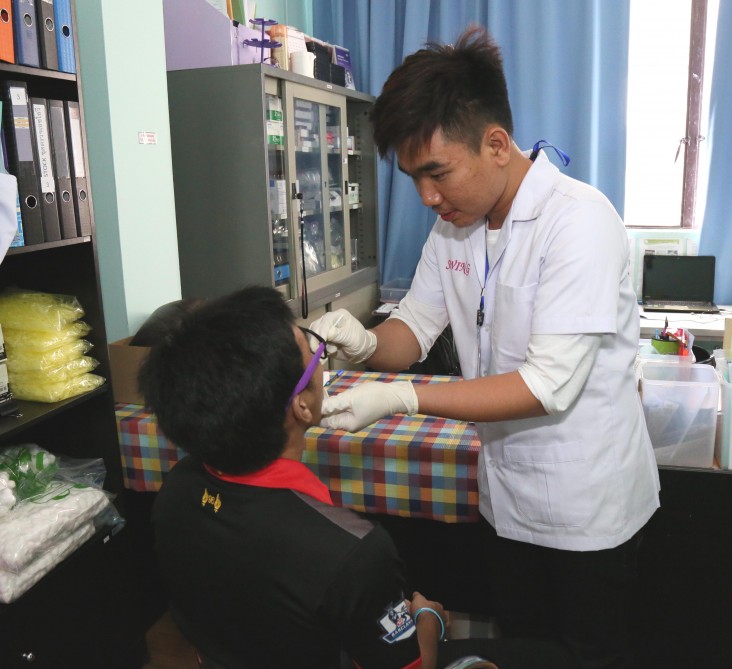
 Dusit Meekrua, right, prepares to conduct a finger-prick test at the SWING drop-in center. “Every time I provide counseling service, I feel like I’m helping someone in my own family,” she says.
Richard Nyberg, USAID
Dusit Meekrua, right, prepares to conduct a finger-prick test at the SWING drop-in center. “Every time I provide counseling service, I feel like I’m helping someone in my own family,” she says.
Richard Nyberg, USAID
 Dusit Meekrua, right, prepares to conduct a finger-prick test at the SWING drop-in center. “Every time I provide counseling service, I feel like I’m helping someone in my own family,” she says.
Richard Nyberg, USAID
Dusit Meekrua, right, prepares to conduct a finger-prick test at the SWING drop-in center. “Every time I provide counseling service, I feel like I’m helping someone in my own family,” she says.
Richard Nyberg, USAID
Speeches Shim
BANGKOK—The old saying, “You are what you eat,” doesn’t apply that well to Atachai Phunkron. It’s more about what he wears. Who would have thought a nondescript lab coat could change his life? Just ask him about it and watch him beam.
“Every time I wear the coat, I feel like it has a magical spell,” said the 28-year-old HIV counselor from Ubon Ratchathani in northeast Thailand. “I feel like I am playing another role—that I commit to transfer knowledge to my clients to save their lives. I used to see people wearing a white coat helping people in the hospitals and had never thought I would have an opportunity to be like them one day.”
It’s a bit unusual that he wears the coat at all given his bachelor’s degree in management from Thailand’s Ramkhamhaeng University. His career aspirations changed when he moved from a sales position to become an accountant for the local NGO, Service Workers in Group (SWING), working in Bangkok and the coastal town of Pattaya. It didn’t take long for him to figure out that he had a knack for helping people.
“I didn’t know if it was because of my fate or my gift, but clients at SWING always came in to consult me about their health and life problems,” he said.
Without a background in health, he took on the challenge and started reading everything he could get his hands on at SWING. His boss, seeing his potential, sent him for training at the Thai Red Cross AIDS Research Center where he learned how to provide counseling services, collect samples, read blood results, provide care support and refer clients to hospital.
Over the past five years, he has provided services to more than 500 clients, of which 90 are HIV-positive. He’s part of a growing and energetic cadre of approximately 150 community activists and caregivers supported by USAID in the past year alone who are rising up to meet key groups of at-risk people—men who have sex with men (MSM), transgender people and sex workers—where they are, and encourage them to be tested.
Through mobile clinics and outreach on-site and online, they bring a friendly face and a warm welcome so those who want to be tested at community centers feel safe and understood. It’s proving to be the best approach to stopping HIV and AIDS in Thailand, with lessons for neighboring countries as well.
SWING is one of seven community-based organizations in Thailand funded by USAID under the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) that is helping reach out to people at risk of getting HIV.
Its staff help conduct an HIV “test and treat” study by the Thai Red Cross AIDS Research Center that, with USAID support, will enroll up to 6,000 Thai men who have sex with men and transgender people from community-led drop-in centers in Bangkok, Chiang Mai, Chonburi and Songkhla.
The estimated prevalence of HIV infection among MSM in Bangkok is 24 percent, and yet only about one-third of MSM have had an HIV test in the past year. In addition, transgender women face particularly high HIV infection risks—49 times higher than the general population, and an estimated 19 percent of transgender women are infected with HIV globally.
Now well into the pilot phase with 1,300 people enrolled, test and treat is showing results.
About 17 percent of all participants are HIV-infected, noted Michael Cassell, USAID’s regional HIV adviser. “It suggests that these efforts are reaching the populations in which they have the greatest benefits,” he said.
About 70 percent of those who have been diagnosed in the study are already receiving lifesaving treatment. National program data suggests that, in the past, fewer than half of men who have sex with men diagnosed with HIV have sought out and received treatment in public facilities.
Early access to HIV treatment can reduce the likelihood of sexual transmission of HIV by more than 95 percent. “Research conducted in partnership with Thailand has armed us with a vision to end the AIDS epidemic by expanding access to antiretroviral medications,” Cassell added. “Now we need communities to lead the charge in reaching and engaging key populations in care.”
Under this community-led approach, community-based organization (CBO) staff provide HIV testing and counseling, explains Dr. Nittaya Phanuphak, chief of the Prevention Unit, Thai Red Cross AIDS Research Center. “With active efforts over the past three years, we have been able to demonstrate that this is feasible,” she said. So far, 10 CBO staff members were trained, and are now qualified to conduct testing, including taking finger-prick blood samples, interpreting results and counseling clients.
In October 2014, Thailand became the first country in Asia to adopt a policy of providing free immediate antiretroviral treatment to all HIV-infected citizens. The test and treat model is taking HIV services to the next level by including pre-exposure prophylaxis (PrEP), a proven new medication to prevent HIV infection among people at risk of contracting the virus.
To scale-up the use of PrEP, the Red Cross has leveraged support from the royal family through donations from Princess Soamsawali Kitiyakara’s fund. With additional USAID support under PEPFAR, the Thai Red Cross AIDS Research Center will benefit from the royal fund and in January launched a three-year project to reduce HIV infection by providing free PrEP to 1,000 MSM and transgender women a year.
PrEP, which is available for under $1 a day at the Red Cross’ Anonymous Clinic in Bangkok, is already attracting interest by doctors and CBO leaders in such countries as Australia, Indonesia, Malaysia, Singapore and Vietnam.
“HIV testing and PrEP is key for Thailand at this moment to be able to visualize the ending AIDS goal in one and half decades from now,” said Phanuphak. “I couldn’t see how we could do that without the involvement of communities and expansion of the community-based model.”
Prapat (not his real name), a 21-year-old MSM, is a believer in PrEP. As a research participant, he takes one pill a day and so far has not experienced any side effects. He remains committed to continue the course and be tested for HIV again within six months.
“I think this is a very good program that reaches the right group of people at high risk like me who need information about how to protect ourselves and other people from getting HIV,” said Prapat, who asked not to be named. “The program should be supported and expanded. If the Thai government would provide more community clinics like this, I think more people would find it comfortable and convenient to get HIV tested and treatment.”
The community-led approach goes a long way to reduce stigma.
“People most at risk of becoming infected with HIV are reached by sympathetic peers, often MSM or transgender people within the community who often prefer not to visit traditional medical facilities for fear of discrimination,” said Beth Paige, director of USAID’s Regional Development Mission for Asia. “PrEP costs less for governments to buy than lifelong HIV treatment, so PrEP should prove cost-effective in the long run if it is targeted to those facing the greatest infection risks. It’s a wise investment.”
To truly roll out PrEP and other HIV services across Thailand and beyond, more community champions need to earn the right to wear white lab coats, just like Atachai Phunkron. He remembers the skepticism of his mother, who first spotted the garment when cleaning his closet—and the joy he had when he presented it and his prized Red Cross certificate to his family back home.
“She told my father, my grandmother and everyone in the family that I was helping people, that I could now speak ‘doctor language’ and that I know about medicine,” he said. “The white lab coat I wear really changed my life, and I pay it the high respect it deserves.”






Comment
Make a general inquiry or suggest an improvement.